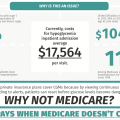
The dangers of competitive bidding for diabetes care and what you can do. Plus, win a year’s worth of any brand of test strips!
Insurance
29 readers recommended
We ask ACA expert Dr. Jack Lord all the hard questions on healthcare coverage and reimbursement.
36 readers recommended
Making sense of Medicare, CGMs, and why it matters to everyone living with diabetes.
45 readers recommended
How fast are insulin prices actually rising? Why might this be happening, and what is the impact on patients with varying levels of health care coverage?
28 readers recommended
What efforts are currently being done to support CGM access?
37 readers recommended
Enrollment period now open until January 31 – our guide to navigating the complex world of health insurance.
44 readers recommended
How sports can be a platform to tackle diabetes awareness and stigma.
40 readers recommended
What to do if you have United insurance.
34 readers recommended
Understanding the UnitedHealthcare/Medtronic partnership in the context of the Affordable Care Act.
32 readers recommended
TCOYD’s CGM Medicare Appeals Assistance Program may be able to help!
33 readers recommended
A run-down on insurance and other payment assistance programs for medical services and prescription medicines
28 readers recommended
What to look for when comparing plans in the healthcare.gov insurance marketplace
41 readers recommended
CGMs with an insulin-dosing claim, like Dexcom’s G5, finally have a path to Medicare reimbursement; possible coverage in 2018 or earlier
51 readers recommended
Lilly announces new program, in partnership with Express Scripts, to provide insulin directly to people with diabetes and high out of pocket drug expenses
42 readers recommended
Cash-pay strips with good accuracy and co-pay programs to save money
28 readers recommended
People with type 1 or type 2 diabetes on intensive insulin therapy can qualify. A major win for the diabetes community following years of patient advocacy!
40 readers recommended
Breaking down employer-based health insurance, employee health benefits, and employee rights for people with diabetes
39 readers recommended
How to get cheaper drugs, find discount programs, get free care in clinical trials, and more
25 readers recommended
How one court ruling may reverse Medicare’s policy denying coverage of most CGMs
27 readers recommended
Acclaimed author James S. Hirsch on his encounter with a broken healthcare system while trying to obtain FreeStyle Libre for his teenage son