Once-Weekly Insulins For Type 1 Diabetes: Latest Research Update

The newest study of once-weekly insulins showed that insulin icodec led to similar reductions in A1C and similar time in range compared to once-daily Tresiba (degludec).
At the 2023 European Association for the Study of Diabetes (EASD) conference, researchers provided an update on the potential of once-weekly insulin icodec for the treatment of type 1 diabetes.
Dr. David Russell-Jones (University of Surrey, UK) presented data from a trial investigating the efficacy and safety of once-weekly insulin icodec compared to once-daily insulin degludec (Tresiba). While several other studies have investigated once-weekly insulins in type 2 diabetes, this was the first data to be presented from a large-scale phase 3 study in type 1 diabetes.
The study, ONWARDS 6, included 582 people with type 1 diabetes who received either insulin icodec or insulin degludec. Participants had an average age of 44 years and an average diabetes duration of 20 years. Both the icodec and degludec group received basal insulin in combination with mealtime insulin (insulin aspart, or NovoLog) over a period of 57 weeks.
Overall, participants treated with once-weekly icodec and once-daily icodec had similar reductions in A1C of -0.5%, suggesting that this new insulin may offer another option for treating type 1 diabetes.
What were the key findings?
This study showed that insulin icodec was effective at reducing A1C in people with type 1 diabetes, although icodec did lead to higher rates of hypoglycemia compared to degludec.
- Average A1C values fell from 7.6% at the start of the study to 7.1% at week 26 in both the icodec and degludec groups, a difference of -0.5%. These results demonstrate that insulin icodec is comparable (or “non-inferior”) to insulin degludec at reducing A1C – notice the two nearly identical lines in the graph below.
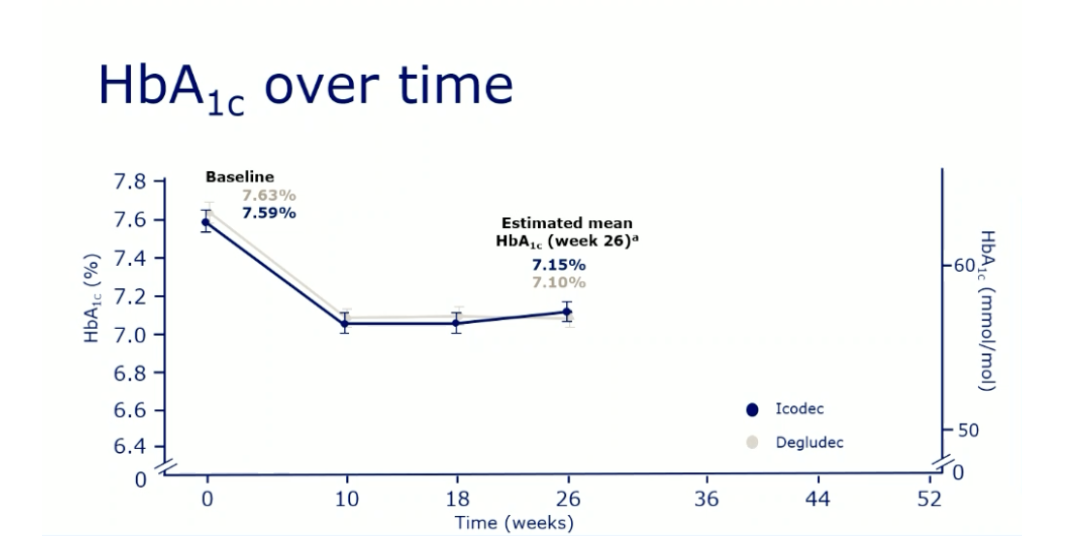
- Time in range (70-180 mg/dL) and time above range (more than 180 mg/dL) were similar between the two groups at both the middle and end of the study, as shown in the graphs below.
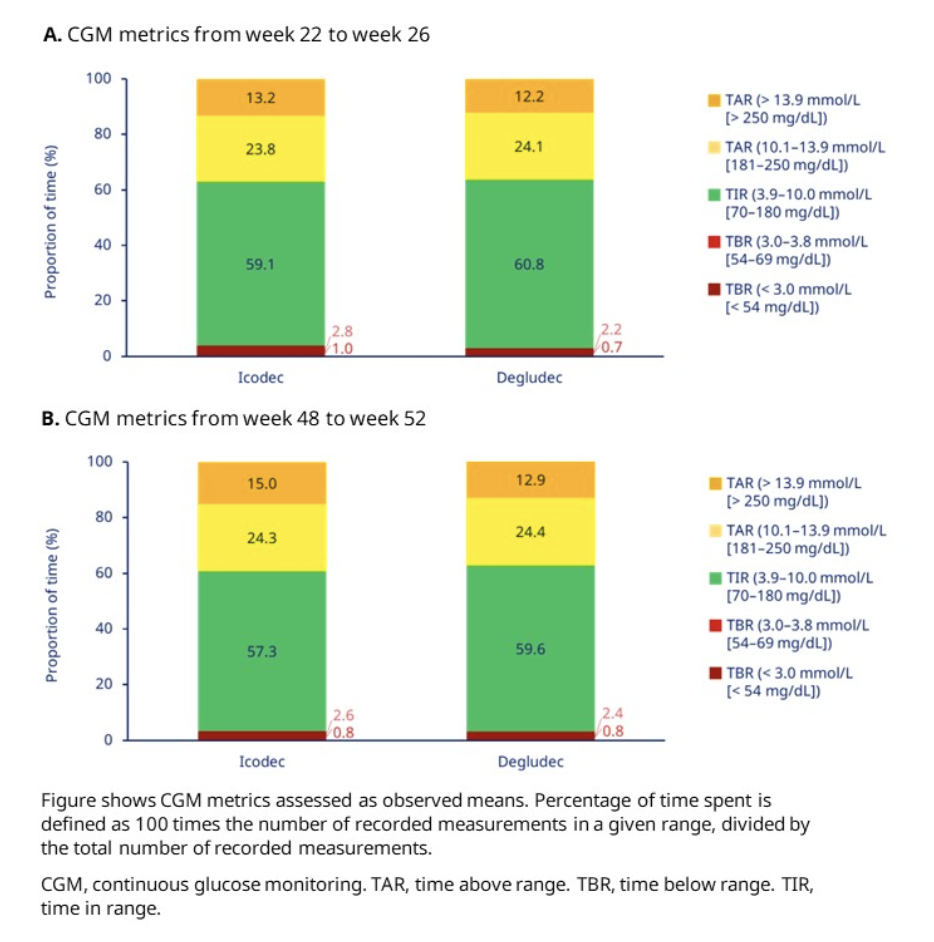
- Hypoglycemia defined as less than 54 mg/dL with CGM was significantly higher in the icodec group compared to the degludec group. Severe hypoglycemia is defined as an hypoglycemic event requiring assistance of another person. The overall rate of combined events of less than 54 mg/dL and severe hypoglycemia was higher in the icodec group with 20 events per patient-year of treatment vs. 10 events per patient-year of treatment for degludec.
- Total weekly insulin dose was similar in the icodec and degludec groups. However, the average weekly basal dose was significantly higher for icodec at 170 units per week (~24 units per day) vs. degludec at 151 units per week (~22 units per day). Meanwhile, the average weekly bolus dose was lower for icodec at 132 units per week (~19 units per day) compared to 161 units per week (~23 units per day) for degludec.
Should people with diabetes be concerned about the higher rates of hypoglycemia with insulin icodec?
While participants on icodec had a higher rate of hypoglycemia compared to those on degludec, Russell-Jones emphasized that these rates are “incredibly low” overall. For comparison, he said that the rates of hypoglycemia ranged from 40 to 80 events for the original clinical trials for Tresiba (degludec).
Researchers are still investigating some questions related to the hypoglycemia events that occurred in this trial, such as how the time of injection and exercise may affect hypoglycemia.
What are the potential benefits of once-weekly insulins?
These results build on preliminary data from June 2022, suggesting that once-weekly insulins may be safe and effective in people with type 1 diabetes.
Reducing the frequency of basal injections could dramatically reduce the burden of diabetes self-management – from 365 injections per year to 52 injections per year. With fewer injections, there is a greater chance that people with diabetes will take their basal insulin consistently. Taking insulin consistently has the potential to improve clinical outcomes, which could reduce the risk of complications like DKA.
Insulin icodec is also being investigated in several different trials in different subgroups of people with type 2 diabetes. Previous research has shown that icodec is just as effective at reducing A1c as once-daily insulin in type 2 diabetes, allowing people to achieve blood sugar targets without experiencing severe hypoglycemia.
Learn more about new insulins in development here: