Diabetes Self-Management Education and Support – Updates and Things You Should Know
By Matthew GarzaEliza Skoler
A new consensus report for adults with type 2 diabetes demonstrates the massive benefits of diabetes self-management education and support programs. Read the recommendations for the four critical periods for DSMES services and hear from the report’s authors
Diabetes self-management education and support (DSMES) programs are led by healthcare teams trained specifically to help people with diabetes set, reach, and maintain their health goals. While you may be familiar with your diabetes educator or CDE, they’re now called diabetes care and education specialists (DCES). These diabetes educators teach people how to check their blood glucose, develop medication routines, incorporate healthy eating and physical activity into their daily lives, and cope with the mental health challenges associated with diabetes. Your diabetes care and educations specialist is there to help you; as a person with diabetes, you have the right to access educational services and support through your healthcare.
DSMES significantly improves blood glucose management as well as the long-term health of people with diabetes. Most insurance plans and Medicare cover DSMES programs with a referral from your healthcare team.
The new DSMES consensus report
A new consensus statement on DSMES for adults with type 2 diabetes was recently published in Diabetes Care and The Diabetes Educator. The report was written collaboratively by many leaders in diabetes, joined by seven national health organizations that included the Association of Diabetes Care and Education Specialists, the American Diabetes Association, and the Academy of Nutrition and Dietetics. While the report was written mainly for primary care providers, it also provides recommendations for policy makers, healthcare professionals, and insurers on how to give the most direct and effective care to people with diabetes.
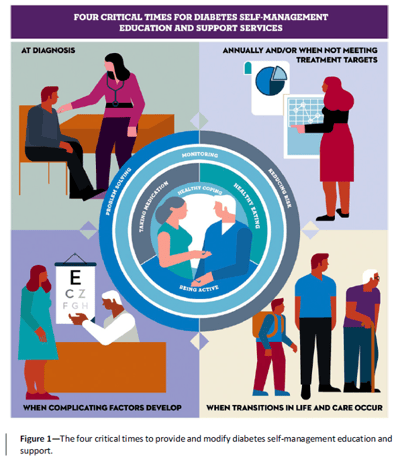
The report emphasizes four important times that people with type 2 diabetes should receive DSMES services:
-
At diagnosis
-
Once a year (or more often) if someone is not meeting their treatment goals
-
If health complications arise
-
When transitions in life and care occur
If you find that you are at one or more of these stages in your diabetes journey, ask your healthcare team about DSMES services! Remember, your care team is there to support you, and you have the right to ask questions and access new services.
Currently, only 5% of people on Medicare receive DSMES and have the opportunity to learn how to safely navigate their diabetes on a daily basis when they are first diagnosed. The goal of this report is to show everyone involved in diabetes care the many benefits people can receive by engaging in DSMES programs as the standard of care (shown in the table below).

Major takeaways from the consensus report
We spoke with the report’s authors, who represent a range of highly respected health leaders, including Joan Bardsley (Medstar), Dixie Harms (MercyOne), Dr. Beulette Hooks (Martin Army Community Hospital), Ellen Mandel (Johnson & Wales University), Dr. Maggie Powers (HealthPartners), and Joanne Rinker (ADCES). They shared with us the most important takeaways from the report, both for people with diabetes and their healthcare professionals.
The authors explained that education may have an important role in improving health trends. When DSMES was compared to metformin as an early treatment option for people with type 2 diabetes, DSMES led to more positive health outcomes than the medication. Specifically, DSMES improved quality of life, increased healthy lifestyle activities, and decreased the risk of health complications. (The table below compares the benefits of DSMES and metformin.)

Dr. Powers told us, “In our recommendations, we say that all people with diabetes deserve the right to have access to diabetes self-management education services. It's part of quality care. You can't just be told to take this medication, or start using the CGM device, or here's a pen, or you need to check your feet every day, or you should cut out your carbs. Somebody has to help with that.” In fact, many healthcare professionals have already started using the report’s suggestions to support people with diabetes in fun and community-oriented ways. In Dr. Hooks’ education group, for example, people with diabetes came together to learn about nutrition, diabetes complications, and exercise; after six weeks, the person with the greatest A1C decline got a prize. The use of DSMES practices like these will promote greater education.
The report also shows the importance of certified diabetes care and education specialists, who are vital to people with diabetes and their healthcare professionals. These educators are some of the most knowledgeable people in understanding and accessing new technologies and therapies, and how to find affordable options for these treatments. Bardsley told us, “It’s really important that [diabetes care and educations specialists] don’t wait for people to come to [them]…we have to utilize the resources that are [in the community] that in many cases may be more trusted because they are within the community.” Successful community-based resources include church gatherings and cooking programs to improve nutrition. Mandel, a physician’s assistant, explained that “reaching out to the community is really essential since diabetes is a full-time endeavor, people with diabetes need to know that they have other people – whether they be peers or religious leaders – that they can lean on.”
In the clinic, healthcare professionals can only provide direct support to people during short appointments. Making sure that a person with diabetes has access to support in their community is vital, whether that be through family and friends or support organizations and community agencies.
The updated consensus report will hopefully make diabetes education more focused on each individual. It provides answers to specific and practical “how, why, and when” questions, as well as specific targets, guidelines, and recommendations. The hope is that healthcare professionals can work with people and their communities to develop goals that address population health and barriers to care.
The rise of telehealth as a response to the COVID-19 pandemic has made it easier for people with diabetes to access educational services. Bardsley said, “So many times access to education [services] is [only] during particular clinic times. So, we need to relook at that because… often people work several jobs. It’s tough to get in to access [these] services for many people. So, hopefully with telehealth, we have more flexibility and we can reach more people.”
The report’s seven recommendations
There are recommendations specifically for primary care providers:
-
Discuss with all people with diabetes the benefits and value of DSMES when they are first diagnosed, as well as after.
-
Provide a referral and support the participation in DSMES at the four critical times: at diagnosis, once a year or more often if not meeting treatment targets, when complications (like heart disease) develop, and when transitions in life and care occur.
-
Make sure that the nutrition plan coordinates with the overall diabetes management strategy – including the DSMES plan, medications, and physical activity
-
Identify and address barriers affecting participation with DSMES services.
The report also includes recommendations for policy leaders, insurance companies, and health care teams:
-
Expand awareness, access, and use of innovative and nontraditional DSMES services.
-
Identify and address barriers influencing healthcare professionals’ referrals to DSMES services.
-
Encourage financial support for DSMES services, given its benefits.
What can you do?
Many people with diabetes do not know about DSMES and the benefits it could have for them and their healthcare team. Dr. Powers laid it out: “We want to empower [people with diabetes] to have a voice to say, ‘Hey, I heard about this. I need a DSMES prescription. I need a referral for Diabetes Self-Management Education.’”
While the DSMES report is written for healthcare professionals, it also shares key lessons for people with diabetes. It is important for your healthcare professional to bring up DSMES services in your appointments, but this may not always happen. We encourage you to share this article and talk with your healthcare team about DSMES and how it may help you or other people in your life.
To learn more about the DSMES report and access additional resources, click here. You can also read more in diaTribe's 2018 article.









