How Sweet It Is: All About Artificial Sweeteners and Diabetes

What are artificial sweeteners, can people with diabetes consume them, and why are they controversial? Here we share advice and break down the types of sugar substitutes that are currently available
You may feel like you’re not sure how artificial sweeteners affect health or relate to diabetes – that’s fair, because there’s a lot of uncertainty on the subject. More than a dozen different kinds of artificial sweeteners are available. These products – also known as low calorie sweeteners, nutritive or non-nutritive sweeteners, or sugar substitutes – help make food and drinks sweet, without the calories found in sugar or the glucose spikes.
So, what are artificial sweeteners? How do they work? How do they affect people with diabetes? And ultimately, are artificial sweeteners good for you?
In short, artificial sweeteners can be much sweeter than sugar itself, so a little goes a long way. This can help reduce how many calories you consume from an artificial sweetener. Additionally, artificial sweeteners are typically not absorbed by the body the way sugar is, so they pass through you without as much concern for weight gain or blood sugar fluctuations.
In this article we’ll discuss what makes one artificial sweetener different from another, their side effects, whether they are safe or unsafe, and how to decide if an artificial sweetener is right for you.
“In our world of diabetes, [these products] make healthy eating more flexible, and they do not take away from one’s daily carbohydrate allotment,” said Toby Smithson, a registered dietician nutritionist and certified diabetes care and education specialist, and the founder of DiabetesEveryday.com. Smithson presented a seminar, “The Sweet Truth about Low Calorie Sweeteners,” at the virtual 2020 conference of the Association of Diabetes Care & Education Specialists (ADCES). Smithson has lived with diabetes for more than four decades and has watched artificial sweetener options grow. She is also a consultant for Splenda, a type of artificial sweetener.
A Bad Reputation
Despite how much they can help with blood glucose management, misperceptions about artificial sweeteners live on. For one thing, while artificial sweeteners themselves have few carbohydrates or calories, the foods they are in likely have some calories and carbs from other ingredients. “Claims like ‘sugar-free,’ ‘reduced sugar’ or ‘no sugar added’ are not necessarily carbohydrate-free or lower in carbohydrate content than the original version of the food. For this reason, we recommend that you read the nutrition facts label to understand how many carbs and calories you are eating,” states the American Diabetes Association’s website. “Using sugar substitutes doesn’t make an unhealthy choice healthy. It just means it’s less unhealthy.”
The Academy of Nutrition and Dietetics, the American Heart Association and the American Diabetes Association have all issued statements indicating that people can use artificial sweeteners cautiously when eaten as part of a healthy diet guided by current federal nutrition recommendations. In her presentation, Smithson said, “The expert consensus on low calorie sweeteners found low calorie sweeteners to be safe, they reduced sugar and energy intake, and had no adverse effects on sweet preference, appetite, or glucose control. Artificial sweeteners may improve diabetes management, but there hasn’t been enough data on gut health and artificial sweeteners to comment on that aspect.”
Still, negative perceptions linger. “Studies on certain sweeteners have revealed questions about their safety which have not been adequately answered,” said Dr. Robert Lustig, author of the upcoming book Metabolical: The Lure and the Lies of Processed Food, Nutrition, and Modern Medicine. “Two examples are aspartame and saccharin, which have been associated with cancer in animals. But these have not been proven in humans. Nonetheless, these doubts persist in the public’s mind.” Lustig argues that we don’t know enough about how sweeteners affect humans to determine whether they are fully healthy for our bodies.
One woman with diabetes came to see Smithson for nutritional guidance and explained that she drank sugary – not artificially sweetened – soda regularly. “She thought it was safer to do,” said Smithson. “To help her understand this, I explained how a regular soda would affect her blood sugar. We suggest drinking regular soda to help spike a blood glucose level within 13 minutes, as a treatment for hypoglycemia. It really got the point across to my patient.”
Today’s Sugar Substitute Options
Why would someone with diabetes think a Coca-Cola would be a better choice than a Diet Coke? With many different products on the market and varying news and studies about nutrition, it can be hard for the public to keep up with changing trends. Similarly, different artificial sweeteners have specific aftertastes, some more obvious than others.
“Some people will use eight teaspoons of sugar in a cup of coffee, and for them it would be hard to transition to an artificial sweetener immediately,” said Sandra J. Arevalo, a dietician, certified diabetes care and education specialist, and National Spokesperson for the Academy of Nutrition and Dietetics. She has counseled people with diabetes over the past 25 years. “I tell them to start reducing the amount of sugar, instead of switching immediately. To reduce the amount of sugar helps change the taste buds, which makes it easier to adapt” to using a smaller amount of an artificial sweetener.
What are the sweeteners available, and what do we know about them? This chart shows common artificial sweeteners that people use at home. All of them are low-calorie, low-carb sweeteners.
Comparison Chart of Artificial Sweeteners
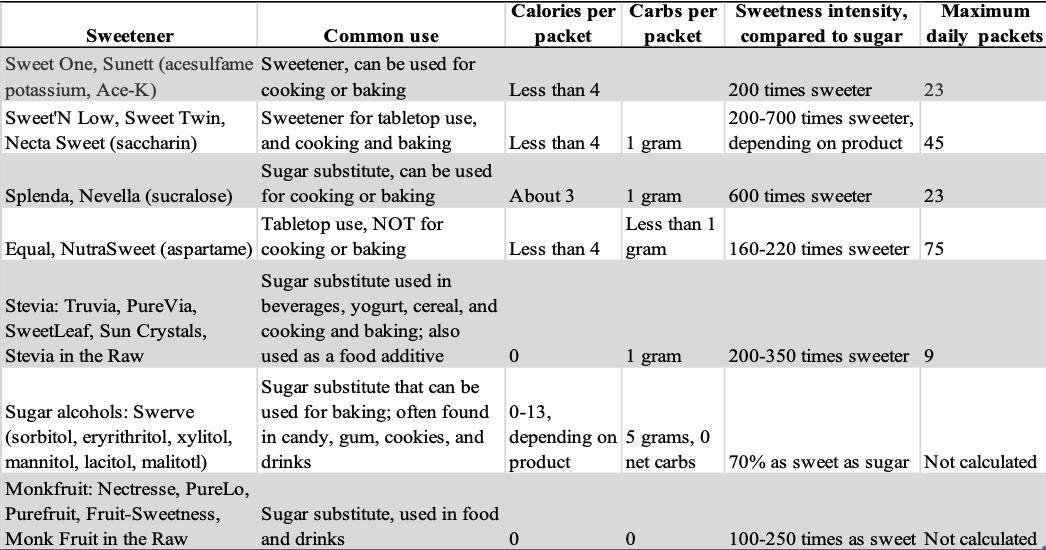
Some artificial sweeteners are mainly used in processed foods. If you’re checking for sweeteners on a food’s nutrition label look for the types listed above, as well as neotame and advantame – two more sweeteners that are thousands of times sweeter than sugar.
Overall, experts recommend using the smallest amount of any sweetener possible. “These sweeteners are safe on a single-dose basis; none of them will make you keel over and die,” said Lustig. “But the question is, what about multiple doses? It’s like tobacco smoke. One cigarette won’t kill you, and not even a pack of cigarettes in one day will kill you. But a cigarette a day for 20 years just might.”
Arevalo agrees.
“Just keep it to the minimum,” she said. “Enjoy it, but be careful of the amount.”
Are some sweeteners healthier?
Some people may be sensitive to certain artificial sweeteners, and Arevalo said plant-based sweeteners may cause fewer side effects such as stomach discomfort.
- Stevia: Stevia sweeteners are plant-based and newer, and they cost more than sweeteners that have been on the market longer, notes Arevalo.
- Monk fruit: “Monk fruit is gaining popularity due to consumer demand for ‘natural foods’ because it originates from the pulp of the fruit,” said Smithson.
Sugar alcohol sweeteners occur naturally in foods and are absorbed by the body more slowly than sucrose. They may be not calorie-free or carb-free, said Smithson. Typically used as a food additive for sugar free candies, cookies, mints and gum, sugar alcohols don’t cause cavities or a rapid jump in blood glucose levels, but they can cause diarrhea, stomach cramps, gas and bloating in some people, especially if you eat a lot of them. Swerve is a sugar alcohol sweetener that is popular among people eating very low carb diets – it has no calories and no effect on blood glucose, Smithson said.
So, which artificial sweetener is best?
Lustig noted that 2017 research published in the Canadian Medical Association Journal found that some studies suggest a possible link between using artificial sweeteners and weight gain and higher risk of obesity, high blood pressure, metabolic syndrome, type 2 diabetes (the studies included people with and without diabetes) and heart disease. However, more research is needed for definitive results.
Lustig’s bottom line is the less sweetness, the better. “Everyone needs to de-sweeten their lives, especially people with diabetes,” he said.
But many people love sweets. With any sweetener, both Smithson and Arevalo recommended that people conduct their own taste test to determine which product they like best, as some sweeteners have a bitter aftertaste. “Everyone’s taste buds are different and everyone’s feelings are different,” Smithson said. “Taste goes a long way and taste matters.”