Does Intermittent Fasting Help People with Diabetes?

Key takeaways:
- Intermittent fasting is a meal schedule that involves alternating between periods of eating and abstaining from food.
- At a session at the 2024 American Diabetes Association conference, researchers discussed the potential benefits of intermittent fasting for diabetes including weight loss, improved insulin sensitivity, and better glucose management.
- Close monitoring of glucose levels and appropriately adjusting insulin doses are crucial when fasting, especially for people with type 1 diabetes who are at higher risk for hypoglycemia and diabetic ketoacidosis.
A big part of living with diabetes means making sure you are eating foods that help keep blood sugar and insulin levels in balance. Of course, this is easier said than done, especially for people who live in areas where access to nutritious food is limited.
Beyond glucose management, getting regular exercise and eating a healthful diet is important for maintaining a healthy weight; living with excess weight or obesity has been shown to increase the risk of developing diabetes or make existing diabetes worse.
This is why researchers, healthcare professionals, and people in the diabetes community are so focused on when (and when not) to eat. Enter, intermittent fasting.
What is intermittent fasting?
Intermittent fasting (IF) refers to a style of eating in which you alternate between a normal eating schedule and consuming little to no calories for a period of time (it could be a few hours or a full day).
While IF might sound restrictive, there are many different ways to do it, depending on what works best for your lifestyle and health needs. All IF eating patterns aim to reduce the number of calories you consume, which can be a huge benefit for people trying to lose weight or maintain weight loss.
Some popular types of IF include:
- Alternate day fasting: As the name implies, you fast every other day. On your fasting day, you consume very little food (500-700 calories or less) and the next day you eat like you normally would.
- The 5:2 plan: This is where you maintain your normal eating schedule for five days and fast for two days. These two days don’t have to be consecutive; for example, you could fast on Tuesdays and Fridays and eat regularly on the other days.
- Time-restricted eating (TRE): This is similar to intermittent fasting, but with a key difference: you fast for a specific portion of the day, but not the entire day. A common approach is the 16:8 method where you restrict the eating window to eight hours a day and fast for the remaining 16 hours. Some people with diabetes, like Justine Szafran, have found TRE to be extremely helpful as part of a daily routine for diabetes management.
- Fast mimicking diet (FMD): This is where you maintain a low-calorie diet for five days of the month and eat normally the rest of the time. Technically, FMD isn’t the same as IF as there’s no actual fasting period, but the period of low-calorie consumption “tricks” the body into feeling like you’re fasting.
Benefits of fasting for diabetes
“Why would we consider the possibility of fasting for people with diabetes?” said Dr. Lisa Chow, director of the Division of Diabetes, Endocrinology and Metabolism at the University of Minnesota, at the 2024 American Diabetes Association conference.
“When you look at the eating window, about 50% of people ate greater than 15 hours and really only stopped when they were asleep. In short, people are eating all the time,” she said.
Overeating is common, especially in countries like the U.S. where portion sizes are larger and unhealthy foods are much easier to access than healthy foods. Finding ways to lower calorie intake, like IF, could help prevent the development of chronic conditions like diabetes.
“If we could reduce basic overeating habits we have in the U.S. we could eliminate a lot of consumption of what's been called ultra-processed food,” said FDA Commissioner Dr. Robert Califf.
Consistently consuming such foods, which are stripped of many vital nutrients during processing, raises the risk for diabetes, obesity, heart disease, and other health problems. Since ultra-processed foods are high in calories and added sugar, they can make blood sugar management much harder for people with diabetes and increase the risk of diabetes-related complications.
Dr. Mark Mattson, a neuroscientist at Johns Hopkins University who has studied fasting for more than 25 years, said our bodies have evolved to handle extended periods without food. In modern times, however, many people have access to high-calorie foods around the clock and can snack all day long – which he believes has contributed to obesity rates and the prevalence of type 2 diabetes. His research suggests that fasting could reverse this trend.
Here’s a closer look at the potential benefits of intermittent fasting.
Encourages weight loss
A growing body of research supports intermittent fasting as a helpful method for weight loss. For example, a small 2022 study found that people with type 2 diabetes who tried time-restricted eating experienced significant weight loss.
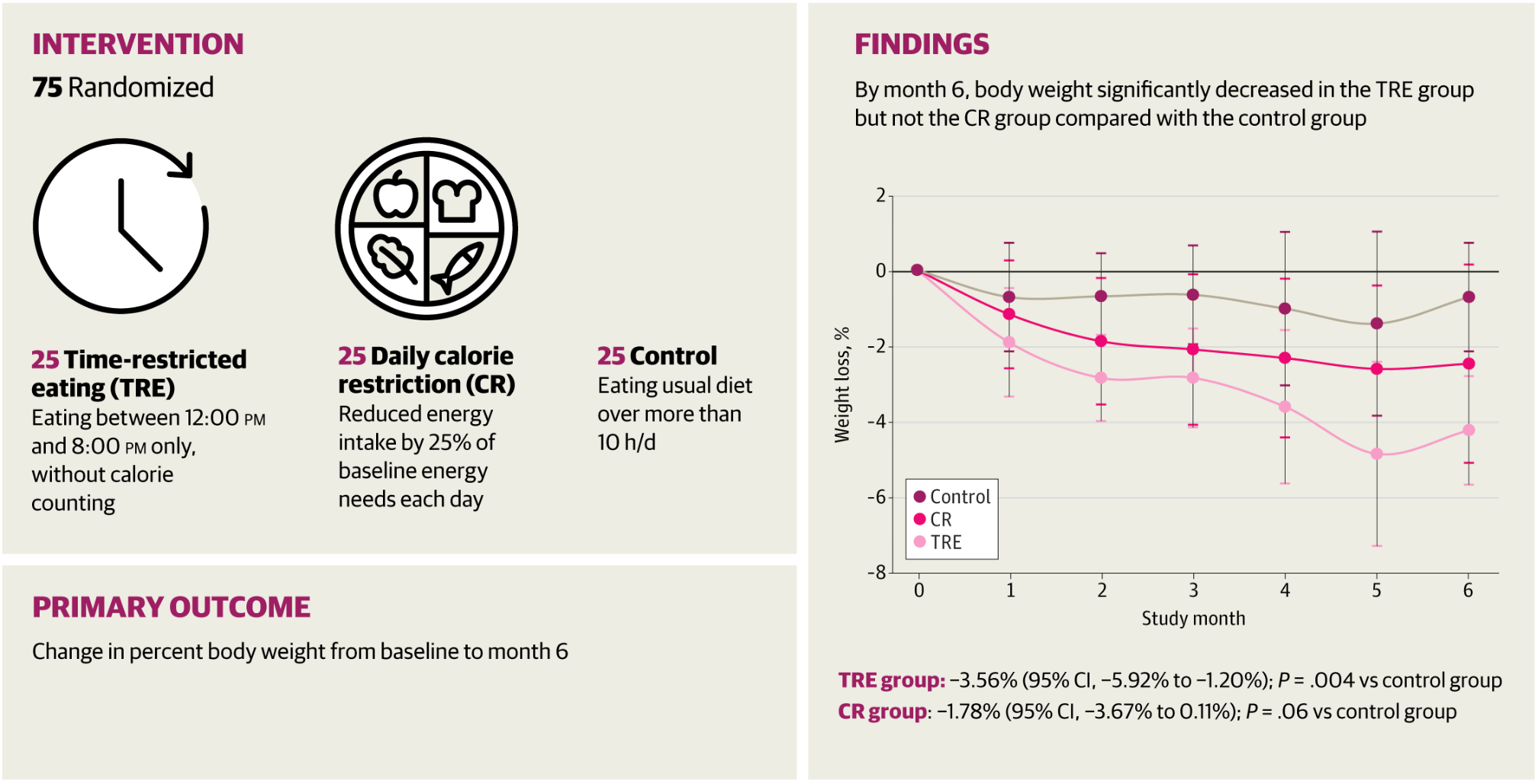
While data on IF for weight loss in the type 1 population is sparse due to the risks for hypoglycemia and diabetic ketoacidosis (DKA), Chow said IF also shows potential for weight loss in type 1 diabetes.
Improves insulin resistance
What does fasting have to do with insulin? Insulin is the primary hormone our bodies use to regulate blood glucose. Maintaining stable blood sugar levels is an important goal for people with diabetes and is often measured by time in range, A1C, and fasting glucose levels.
A 2021 review showed that individuals who practiced IF had a significant reduction in fasting glucose levels with an average decrease of 4 mg/dL. Other important findings included a reduction in A1C levels, weight loss, and an increase in adiponectin (a natural hormone shown to increase insulin sensitivity). Numerous other studies, including a large 2022 review, list improved insulin resistance as one of the many benefits of IF.
Helps balance blood sugar
IF also shows promise as a useful tool for blood sugar management. One study testing IF in people with type 2 diabetes observed significant reductions in A1C levels and body weight after 12 weeks.
A 2024 review on time-restricted eating showed similar findings, with fasting resulting in decreased A1C in those with type 2 diabetes. Though improvements in glycemic control are suggested to be a result of weight loss (a healthy weight is associated with better blood sugar levels), the results are meaningful nonetheless.
How exactly does intermittent fasting work?
Sugar and fat serve as our body’s main sources of energy. After a meal, sugars are used for energy first. They are broken down and delivered to the bloodstream, while fats are stored for energy later. When we restrict eating, our bodies run out of carbohydrates to use for energy and instead break down stored fats, converting them into ketones.
During fasting or carbohydrate restriction, the body uses ketones for energy as glucose runs out. The change from using sugars to ketones is known as metabolic switching, a process that scientists suggest produces many of the health benefits attributed to fasting. IF allows people to manage this process of metabolic switching.
Is intermittent fasting safe for people with diabetes?
“Prolonged fasting is possible and likely safe in the setting of type 1 and type 2 diabetes,” said Chow.
Of course, this comes with caveats, she said. The excess production of ketones from IF can lead to a dangerous condition known as DKA – a major concern for those with type 1 diabetes. Risk factors like this, along with hypoglycemia, are big reasons why IF research in this community is tricky.
But that doesn’t mean those with type 1 diabetes can’t try IF. In fact, many do. In a 2024 survey of people with type 1, 30% reported participating in some type of fasting program, with time-restricted eating being the most common.
More research is needed, but small studies have found people with type 1 diabetes who have well-managed diabetes can successfully fast with limited risk for severe hypoglycemia. That said, there are some steps people with diabetes – specifically type 1 – need to take to fast safely.
“Both IF and TRE will drop a person’s glucose levels, meaning that medication adjustments are necessary to avoid hypoglycemia during the period of calorie restriction,” said Dr. Robert Ratner, a long-time scientific and medical leader in diabetes. “Changes in eating patterns on a daily basis will also require medication adjustments to keep glucose levels in range.”
Along with carefully monitoring glucose levels to avoid low blood sugar episodes, insulin must be appropriately reduced during fasting periods. Since insulin is essential to avoid DKA, dosing adjustments must be done cautiously.
Since IF also increases ketone levels, it’s important to regularly test ketone levels to avoid the risk of DKA. You can easily test ketones using an at-home urine test or blood glucose meters that also test ketone levels.

The same risks for hypoglycemia apply to people with type 2 diabetes who are fasting. IF appears to be most safe for those who do not need glucose-lowering medications. It’s always a good idea to talk to your healthcare team before fasting, especially if it’s your first time trying it.
Drawbacks of intermittent fasting
Although IF is shown to have health benefits and is generally safe for many people with diabetes, there are some drawbacks to consider. Besides risks for hypoglycemia and DKA, fasting may cause side effects such as:
- Dizziness
- Headaches
- Hunger
- Increased heart rate
- Irritability
- Shakiness
- Sweating or chills
Another difficulty is changing your eating habits (cut yourself some slack here, starting a new routine of any kind is hard). Transitioning from eating whenever you want to planned fasting can be stressful and might not align well with your daily life. For example, if you exercise in the morning or are an athlete, it might not be possible to engage in these activities on an empty stomach.
IF also can lead to unhealthy eating habits, including disordered eating. If you are concerned that you or someone else with diabetes may be experiencing disordered eating, contact the Diabulimia Helpline. The National Eating Disorders Association is another great resource for anyone with or without diabetes.
Expert tips for a healthy fasting experience
Although you can use IF in several different ways, there are specific steps to take to ensure it’s successful for weight loss, diabetes management, or whatever your health goals are.
“The health benefits of IF are due to calorie reduction. If people overcompensate when they are eating, the impact is lost,” Ratner said.
If you decide you want to pursue some sort of intermittent fasting plan, here’s what to keep in mind.
- Staying hydrated is critical. During fasting periods, you can drink water or unsweetened, zero-calorie beverages. Black coffee or tea are great options as these beverages can help suppress appetite and curb cravings.
- Start slow. A 16:8 time-restricted eating might be easier to incorporate into your daily schedule than intermittent fasting because it gives you the chance to build a regular eating schedule every day.
- It might be uncomfortable, but remember, it’s okay to feel hungry. More intense food cravings may be experienced at the beginning of a fasting period, but your body is adaptable and will get used to the new eating pattern. Some people even experience a boost in energy after they get past the initial hunger.
- If you have access, use a continuous glucose monitor (CGM). A CGM can be immensely helpful for you (and your healthcare provider) to measure changes in glucose levels before, during, and after fasting.
- Make sure to get enough rest. Don’t force yourself to do strenuous activities or hardcore exercise on fasting days. Your body isn’t getting the same levels of glucose it normally uses for energy, so don’t feel guilty about taking it easy – it’s okay (and encouraged) to relax.
- When beginning a fast, monitor yourself for side effects. Start a journal where you can record your feelings and experiences for future reference and discuss them with your healthcare team.
- When resuming your regular eating routine, IF does not require you to adhere to any specific food plan. However, it could be helpful to make a meal plan for non-fasting days to make sure you’re eating foods best for your health. For people with diabetes, it’s best to consume natural, nutrient-rich whole foods that are not likely to spike your blood sugar.
- Consult your healthcare provider before making any significant changes to your diet or medications. If they agree it’s safe for you to try a new eating pattern like IF, they can advise you on how often to monitor glucose and whether you’ll need to adjust your insulin dosing or other medications.
Remember: it’s okay to miss a day of IF – that doesn’t mean you’ve failed. Similarly, it’s okay if intermittent fasting is not for you. There are lots of other lifestyle changes to help you manage your diabetes successfully.
The bottom line
Intermittent fasting is a viable alternative for people to reduce calorie consumption over time. While research on IF is limited in populations with diabetes (especially type 1), a growing body of evidence shows promise for it as an effective tool for weight loss, blood sugar management, and improving insulin sensitivity.
There are many different ways to fast, making it a fairly flexible eating plan that you can adjust based on your individual needs and health goals. While IF can be safe for many people with diabetes, it can increase the risk of hypoglycemic events – especially in individuals taking medicine to lower blood sugar levels. It also poses a risk for DKA in people with type 1 diabetes, which is why it’s critical to closely monitor blood sugar levels and reduce insulin doses as necessary to avoid hypoglycemia.
For anyone with diabetes, talk to your healthcare provider before trying IF to determine if it’s safe for your health and well-being. Never stop taking diabetes medications or change the dosage without consulting with a healthcare professional first.
Learn more nutrition and diets for diabetes here: