So You Got a CGM – Now What?
 By Katie Mahoney, Hanna Gutow, and Diana Isaacs
By Katie Mahoney, Hanna Gutow, and Diana Isaacs
If you just got a continuous glucose monitoring system, you may be wondering how to use it most effectively and how to understand your glucose data. Read our tips, tricks, and things to consider.
Congratulations – you got a continuous glucose monitor (CGM), an excellent tool to support diabetes management. Hopefully you’re feeling optimistic and excited that you have the opportunity to use this technology.
It’s most likely that you and your healthcare team decided that using a CGM is the optimal way for you to manage your diabetes. Perhaps you were given a prescription for a personal CGM. Or maybe you’re trying CGM as part of Dexcom’s Hello Dexcom program (a free ten-day trial), through Abbott’s MyFreestyle program (a free 14-day trial), or as part of Medtronic’s CGM Discount Access program. You might also be trying professional CGM, which is owned by your healthcare clinic and worn on a short-term basis.
If you haven’t yet been able to get CGM, ask your healthcare team if you can get a trial device or get a prescription. CGM is recommended for anyone with diabetes who takes mealtime insulin. While many people with diabetes currently don’t have access to CGM, we’re hopeful that more and more individuals will be able to use this technology in the future. Regardless of what brings you to using a CGM, we’ve created a three-part guide to help you get started, including tips, tricks, and considerations.
Click to jump down to a section:
Part 1: Before you apply your CGM
Learn the basics.
Before you start using your CGM, it can be helpful to understand its basic features. Continuous glucose monitors (CGM) measure the body’s glucose (or sugar) levels by sensing the glucose present in tissue fluid (also called interstitial fluid). While a blood glucose meter (BGM) provides a measurement of the blood glucose level at a specific moment in time (when you prick your finger), CGMs provide a new glucose level every one to five minutes – depending on the device, that’s 288 to 1,440 times per day. A CGM provides a constant stream of information on glucose levels, trends, and patterns.
A CGM can either be transcutaneous (it goes through your skin) or implanted (it lies under your skin). CGMs require three basic parts:
-
A sensor that monitors real-time glucose levels under your skin.
-
A transmitter that sits on top of the sensor and sends glucose information to a smartphone app, reader, or receiver. In transcutaneous systems, the sensor and transmitter are connected as one small on-body device. Some transmitters are disposable with the sensor while others require an additional step to attach. In implanted systems, the transmitter is attached to the skin and can be removed without harming the sensor below the skin.
-
A smartphone app, reader, or receiver to collect and display your data.
CGMs have a variety of features that differ by brand and model, including the amount of time the CGM needs to “warm up” before glucose readings are available, how long you can wear a CGM sensor before needing to replace it, and alarms that alert you to highs and lows. You can learn more about CGM devices here. For brand-specific resources and information, click here to jump down.
Personal CGM vs. Professional CGM
The CGMs that we just described are called personal CGMs – they are owned by the person with diabetes and used for a long period of time. They are available as real-time CGMs, where the data can be continuously viewed, or as intermittently-scanned CGMs, where information is recorded all of the time, but you need to scan the sensor to view the data.
Another type of CGM is called “professional CGM.” Professional CGMs are given to someone with diabetes for a short session (usually one to two weeks) to better understand that person’s glucose levels. After the wear period, the person will review the data with their healthcare professional. This can provide insights that inform the person’s diabetes treatment, and it can help healthcare professionals recommend therapy and lifestyle recommendations that lead to better glucose management.
Some professional CGMs have a real-time mode, meaning that the user can see their glucose levels while wearing the device. Other professional CGMs have a “blinded” mode. Blinded CGM means that you cannot look at their glucose values on-demand; instead, all of your glucose data is stored and shared with your healthcare professional. This can help your healthcare team identify hypoglycemia (or low blood sugar levels). If you get a blinded professional CGM, your healthcare team will analyze the data and discuss it with you once your wear period is complete.
While long-term, real-time CGM is most effective for day-to-day diabetes management, especially for insulin users, professional CGM can be an important tool for people who are not using personal CGM. Periodic use of CGM can help people learn the effects of food and physical activity on glucose levels, even for those not taking any diabetes medications.
Reflect on your goals, know your targets, and make a plan to respond to highs and lows.
It can be helpful to reflect on your CGM goals, set your glucose targets, make plans for responding to your glucose readings, and decide with whom you want to share your data:
-
Reflect on your CGM goals. Perhaps you want to use CGM to prevent hypoglycemia using its alert system, or to prevent hyperglycemia and increase your Time in Range, or to manage glucose during exercise. Or, maybe you and your healthcare team are going to use professional CGM for two weeks to explore how your lifestyle habits affects your glucose levels. Regardless, the ultimate goal of CGM is to improve your diabetes management.
-
Know your personal glucose targets and make a plan with your healthcare team for how you’ll respond to hyperglycemia and hypoglycemia. Knowing your target glucose range is important for responding to your real-time glucose values. For most people with diabetes the target range is 70-180mg/dl – learn more about Time in Range goals here. Make a plan that incorporates glucose trend arrows from your CGM to help you prevent big spikes out of range. Here are some prompts for you to discuss with your healthcare team:
-
What is my glucose target when I wake up and before meals?
-
What should my glucose level be two hours after a meal? If it is above that value, what actions should I take to bring my glucose levels down?
-
What is my glucose target before bed?
-
What high glucose level should I try to avoid? What should I do if my glucose gets that high?
-
What low glucose level should I try to avoid? What should I do if my glucose gets that low? What should I do if my glucose levels are trending down?
-
Part 2: Applying your CGM
Connect the CGM to the app and set the system up.
Download the mobile app associated with your CGM system if available. If you’re using a receiver (Dexcom device) or reader (Libre device), make sure it’s charged daily. The CGM should come with instructions for applying the sensor (every seven, ten, or 14 days) and pairing the app, reader, or receiver with your sensor and transmitter. If you have an implanted CGM, it will be applied by a healthcare professional and can last up to 90 days. To jump to brand-specific instructions and tutorials, click here. To learn about CGM adhesives and tips for keeping your CGM on, check out Adam Brown’s suggestions on the topic.
Once your system is set up, your CGM will need to “warm up” before you can see your data. Different models have different warm-up periods, but this will generally take one to two hours, after which your data will be accessible either directly (Dexcom, Guardian, Eversense) or by scanning your sensor (FreeStyle Libre). The warm up period for the implantable Eversense system is 24 hours.
For many people starting to use a CGM, video tutorials can be quite helpful. If you have the opportunity, it’s good to meet with a diabetes care and education specialist or your local pharmacist (if picking up your CGM from a pharmacy). Here are set-up and application tips and tutorials for your CGM:
-
Abbott: FreeStyle Libre 14-day Tutorials
-
Abbott: FreeStyle Libre 2 Tutorials
-
Dexcom: G6 Tutorials
-
Medtronic: Guardian Sensor Tutorials
-
Senseonics: Eversense Tutorials
Part 3: Understanding your CGM data
Once you’re set up with your CGM and the warm up period is complete, you can access your data. There are two types of data you’ll want to pay attention to: real-time data and past data.
Interpret your real-time data.
Depending on the CGM brand you’re using, you can either access your glucose data at any time by looking at an app on your phone, your smart watch, or your receiver. For those using an intermittently-scanned CGM, you can view your glucose levels by scanning your sensor with your smart phone or reader. Looking at your data can feel overwhelming at first, so we recommend focusing on two aspects of your real-time data:
-
First, look at your CGM glucose value. Is it in your target range? If your glucose level is out of range, which steps of your plan should you follow?
If you’re experiencing hypoglycemia in particular, make sure you act right away to increase your glucose levels.
-
Second, look at the trend arrow. Your CGM provides a “trend arrow,” to tell you the direction and speed with which your glucose values are changing. The trend arrow is helpful for understanding what’s going on and how you can respond. For example, if your glucose value is 90 mg/dl and your trend arrow shows that your glucose levels are going down, you may need to take action to prevent hypoglycemia; if your glucose value is 90 mg/dl and your trend arrow shows your glucose levels are increasing, you are likely not going to develop hypoglycemia.
Trend arrows can help with premeal insulin dosing, before and after exercise, before bed, and to understand where your glucose will be trending in the next 30 minutes. Trend arrows are particularly beneficial when used with insulin on board (short-acting insulin that was recently taken for food or to correct a high glucose level and is still working in the body). For example, if your trend arrows are going down and you have insulin on board from an insulin dose given two hours previously, your risk of hypoglycemia is even greater.
For those not using insulin, trend arrows can help understand how different foods and activities affect glucose levels. For example, if a person sees that the arrow is rising rapidly after a certain meal or snack, they can go for a walk to try to bring it down. It may also signal that next time you should consider a smaller portion size or try to add protein or fat to prevent glucose levels from rising as quickly.
Each CGM has a slightly different interpretation of the arrows, but here’s a general idea of what the trend arrows can tell you.

We recommend working with your healthcare team to decide how often to check your glucose levels. Many people benefit from checking glucose when waking up, before meals, before physical activity, and at bedtime. Some people benefit from checking one to two hours after meals. A person should also check their CGM any time they feel symptoms of high or low glucose. CGM alarms are especially helpful for monitoring glucose levels as they change – more on this below.
Interpret your past data.
Once you’ve used your CGM for a few days, you can see your recent daily trends and the amount of time you’re spending in the target range (70-180 mg/dl). This is also called retrospective data. It is beneficial to review your glucose data regularly to understand how your lifestyle – like the food you eat, your exercise habits, your stress levels, and medications you use – affects your glucose levels. Look at your glucose levels over the past two weeks, one month, and three months; talk with your healthcare team about trends that you are noticing and how they might be addressed. Learn about the many factors that affect glucose here.
During diabetes care appointments, your healthcare team can view this data in an Ambulatory Glucose Profile (AGP) report and use it to talk with you about how your diabetes management is going and any potential adjustments to your care plan. This should be a collaborative discussion between you and your healthcare team about how your diabetes data compares to your management goals and what changes could be made.
Each CGM system offers a standardized one-page report, called an ambulatory glucose profile (AGP). The AGP includes three important components:
-
CGM key metrics
-
24-hour profile
-
Daily glucose patterns
Although there are many ways to view your glucose data, the AGP report often has all of the information that you need. We’ll explain the three main pieces below. To learn more, read our in-depth piece on understanding your AGP report: “Making the Most of CGM: Uncover the Magic of Your Ambulatory Glucose Profile.”
CGM key metrics
More green, less red.
The time in range bar shows the percentage of time you spend in five glycemic ranges:
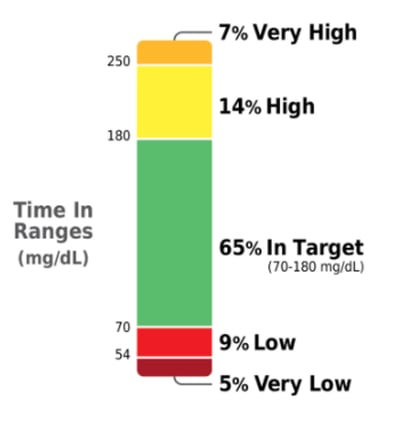
Time in Range: glucose levels between 70-180 mg/dl
-
Time Below Range: glucose levels below 70 mg/dl
-
Time in severe hypoglycemia: glucose levels below 54 mg/dl
-
Time Above Range: glucose levels above 180 mg/dl
-
Time in severe hyperglycemia: glucose levels above 250 mg/dl
Your goal is to grow the green bar and shrink the red bars – in other words, increase Time in Range and decrease time Below Range and time in severe hypoglycemia. See more on Time in Range goals and standard targets.
24-hour profile, also known as Ambulatory Glucose Profile (AGP).
 How do you figure out how to change your diabetes management to increase your Time in Range and decrease your Time Below and Above Range? That’s where the 24-hour profile is helpful, which shows your daily glucose trends across the full 24-hour day.
How do you figure out how to change your diabetes management to increase your Time in Range and decrease your Time Below and Above Range? That’s where the 24-hour profile is helpful, which shows your daily glucose trends across the full 24-hour day.
-
Understanding what the 24-hour profile shows: The black line represents your median glucose level throughout the day based on data from a set period of your CGM use (e.g., the last two weeks). The blue shaded areas help show how much your glucose levels vary at different points in the day.
-
Using the data: Compare different times of day to see what might be influencing your glucose numbers. For example, while the person shown above has glucose readings that vary greatly at 3pm (indicated by a very wide shaded area), their 8am glucose numbers are much more consistent (the shaded area at 8am is narrower), despite being higher. This person also regularly sees a spike in sensor glucose readings at around 9am. What’s causing that increase? Maybe it’s a higher carbohydrate breakfast choice, forgetting to bolus, not bolusing early enough, or not accounting for all the carbs in breakfast. Reflecting on what is causing a spike or valley can help you make behavior changes to reduce fluctuations and increase your Time in Range.
-
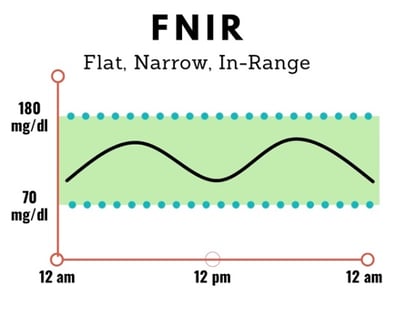 The goal: The overall goal is to keep your glucose levels in your target range without big spikes or valleys, sometimes called “flat, narrow, in range” (FNIR). In the AGP above, the green box represents the user’s target sensor glucose range (70-180 mg/dl). While the user stays in range overnight and in the afternoon, they tend to see spikes in the morning and evening. With the goal of FNIR in mind, you can look at your long-term data and ask, what’s making it possible for me to stay in range? What is making my glucose spike or fall?
The goal: The overall goal is to keep your glucose levels in your target range without big spikes or valleys, sometimes called “flat, narrow, in range” (FNIR). In the AGP above, the green box represents the user’s target sensor glucose range (70-180 mg/dl). While the user stays in range overnight and in the afternoon, they tend to see spikes in the morning and evening. With the goal of FNIR in mind, you can look at your long-term data and ask, what’s making it possible for me to stay in range? What is making my glucose spike or fall? -
The good news is the goal for most people is to spend 70% or more Time in Range. However, increasing your Time in Range by even 5% (an extra hour per day in range!) can be helpful. You don’t have to reach perfection to improve clinical outcomes.
Daily glucose profiles.
With your trend data, you also can see your daily 24-hour glucose profiles from the last two weeks. The figures show the target range (70-180 mg/dl) in gray, spikes above 180 mg/dl (hyperglycemia) in yellow, and valleys below 70 mg/dl (hypoglycemia) in red. Viewing the data day by day can help you evaluate how specific factors and behaviors impacted your glucose values on a certain day.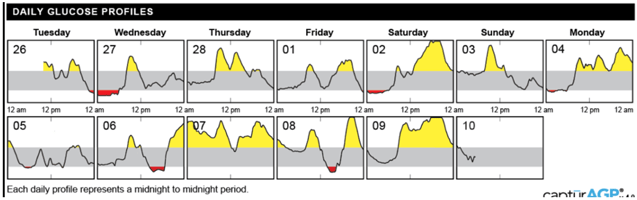
To make the most out of your daily glucose profiles, it can be helpful to log your daily food and exercise to compare with your glucose profile and see which behaviors help you stay in range and which ones tend to make you go out of range.
A helpful tool when reviewing your data with your healthcare team is called DATAA. Which stands for:
-
Data – look at your diabetes data together
-
Assess Safety – Look for and try to solve Time Below Range (hypoglycemia) first
-
Time in Range – Discuss what’s working and how to replicate that by looking for the times of day or the days of the week when Time in Range was the highest
-
Areas to Improve – Note when you spent more Time Above Range (hyperglycemia) and discuss ways to reduce this
-
Action Plan – Develop an action plan together
Other Tips, Tricks, and Considerations
1. Exercise & your CGM
To learn about how to use your CGM before, during, and after exercise, check out our article “Exercise Well with Your CGM – Recommendations, Glucose Trends, and Strategies.”
An important note about exercising with a CGM: There can be a difference between CGM glucose measurements and BGM glucose measurements due to what we call a “lag.” Changes in glucose levels in interstitial fluid are not seen as quickly as they are in the blood. At rest, the interstitial glucose lags about five minutes behind the blood glucose; in situations when glucose changes rapidly, such as during exercise, lag time can increase up to 24 minutes. This means that your CGM readings aren’t always going to be accurate during exercise. This lag can also occur outside of exercise, any time your glucose levels are rising or falling quickly.
2. How to make CGM alarms your friend
Adam Brown has written about how it can be helpful to think about your CGM as a partner in your diabetes management, rather than a nag that points out when you’re not in range. Alarms can be useful tools. By alerting you to current or predicted highs and lows, as well as rate of change, you can increase your Time in Range and see your 24-hour glucose profile become flatter, narrower, and more in range. You can personalize your CGM alarm settings to your preferred thresholds or turn them off completely (though some devices won’t let you turn off an urgent low alarm at 55 mg/dl). It’s helpful to work with your diabetes care team to determine your individualized alarm settings.
3. Sharing data with friends, family, and care-partners
The ability to share your real-time glucose data with your care-partners and loved ones is a huge plus of using CGM – your support network can help you track your glucose levels and keep them in range. At the same time, sharing your data with others makes some people nervous and self-conscious. Decide who you want to share your data with and talk with that person about boundaries and how you want to communicate about your data. For more on how to approach these conversations, check out Kerri Sparling’s “To Share or Not to Share: My Approach to Diabetes Data,” and “How to Coach Your Care-Partner on CGM Data.”
4. How to talk to your healthcare team about your CGM
Now that you’re using a CGM, talking with your healthcare team about your CGM data should become a key part of every visit.
Ahead of the visit: To help visits go smoothly, many healthcare professionals will ask you to upload your CGM data before you come into the office (or before your telehealth appointment) so they can review the data and be prepared to talk with you. Learn about uploading your data here. Note: some CGM systems upload automatically once connected to the clinic’s data portal. It’s also helpful to look over your data – like your AGP report – and come up with questions to ask your healthcare professional ahead of the visit. You may have questions about parts of your daily glucose profile that you don’t understand, areas where you’re having a hard time staying in range, or just general questions to help you navigate your data.
During the visit: To make sure that you and your healthcare professional are on the same page, it can be helpful to take a few minutes at the beginning of your appointment to explain your interpretation of your data in your own words. This may be a good time to start a conversation on any questions you may have prepared ahead of your visit. It is also important to take time with your care team to develop an action plan based on your CGM data with a few straightforward priorities for you to focus on before your next visit.
Brand-Specific Resources
While any CGM can help improve your diabetes management, there are some differences between the currently available systems that you may want to consider or talk about with your healthcare team – see our chart comparing different CGMs here. Specifically, we recommend asking your healthcare professional about how alarms may be able to alert you to times of hyperglycemia or hypoglycemia, what it means if you have to calibrate your CGM, and how to use your CGM with smart insulin pens, mobile apps, or even insulin pumps in an automated insulin delivery (AID) system.
To reach out to CGM companies for product support, contact their customer service departments:
-
Abbott: +1-855-632-8658
-
Dexcom: +1-888-738-3646
-
Medtronic: +1-800-646-4633
-
Senseonics: +1-844-736-7348
This article is part of a series on Time in Range.
The diaTribe Foundation, in concert with the Time in Range Coalition, is committed to helping people with diabetes and their caregivers understand Time in Range to maximize patients' health. Learn more about the Time in Range Coalition here.







