Diabetes and Heart Disease – Keep Your Heart in the Right Place
Diabetes and heart disease are closely connected. This article discusses heart disease, important numbers to know, and ways to improve your heart health
A person with type 2 diabetes is twice as likely to have heart disease or suffer from a stroke than someone without diabetes. But there are steps that you can take right now to improve both your diabetes management and your heart health, all at the same time! We teamed up with The American Heart Association and American Diabetes Association’s Know Diabetes by Heart (KDBH) initiative to talk about the best way to keep your heart healthy with diabetes.
How does diabetes affect your heart?
High blood sugar levels can damage the blood vessels and nerves that support your heart. This process occurs slowly over time – the longer you have diabetes, the more likely you are to develop heart disease.
High blood pressure (or hypertension), another common complication in people with diabetes, can also raise the risk of heart disease. High blood pressure means that blood is traveling through your blood vessels with a lot of force. Like high blood sugar, the increased force can damage the walls of your blood vessels.
People with diabetes often have high levels of LDL (“bad”) cholesterol and high triglycerides (a type of fat found in your blood). LDL cholesterol and triglycerides can form plaques (fatty deposits) that attach to blood vessels and thicken their walls, making it more difficult for blood to pass through (this is called atherosclerosis). A heart attack or stroke occurs when an artery is completely blocked, cutting off blood flow. To learn more about how cholesterol and triglycerides affect heart health, watch this short video from the American Heart Association.
What can I do to keep my heart healthy?
Start by talking to your healthcare professional. KDBH recommends the following four top questions to ask your healthcare team:
- What can I do to lower my risk for heart disease and stroke?
- Do any of my medications help me manage my risks for heart disease or other complications?
- Are there programs that can help me manage my condition? Can you give me a referral?
- How can I meet other people going through my same experience?
Download the full discussion guide from KDBH here. Below we'll talk about some strategies that address these questions to keep you healthy.
During the coronavirus pandemic, many people have delayed or postponed their routine medical care in order to avoid overcrowded hospitals and doctor’s offices dealing with people who have COVID-19. It’s important to begin resuming these appointments either in person or through virtual telehealth options, if available to you. That said, you should also take precautions to keep yourself and others safe.
Because people with pre-existing conditions like diabetes and heart disease have more risk of severe complications of COVID-19, it is critical to manage your conditions and keep your numbers within healthy ranges. But what are those “numbers” that you should focus on?
Know your numbers:
Many of the risk factors of heart disease do not have symptoms. That is why it is important to talk to your healthcare professionals and ask them to evaluate your heart health. Knowing these specific numbers will inform you and your healthcare team and help guide treatment decisions; learn more from KDBH.
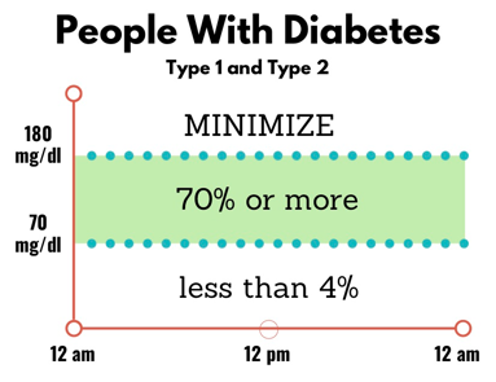
Time in range and A1C: Time in range and A1C will give you a snapshot of your blood glucose management. Experts recommend that most people with type 1 or type 2 diabetes should aim for the following time in range goals:
- At least 70% of the day with blood sugars between 70 to 180 mg/dL
- Less than 4% of the day with blood sugars below 70 mg/dL
- Minimize time each day with blood sugars above 180 mg/dL
A1C is measured with a blood test and provides a snapshot of your average blood glucose levels over the past two to three months. Experts recommend that people with diabetes aim for an A1C of 6.5-7% or lower, as long as people reach this without increasing the risk of severe hypoglycemia or other complications.
Cholesterol and triglyceride levels: Cholesterol and triglycerides are measured with a fasting blood test. It is important to have this done each year, or as recommended by your healthcare professional. Experts recommend:
- Total cholesterol: less than 200 mg/dL
- LDL (bad) cholesterol: less than 100 mg/dL
- HDL (good) cholesterol: more than 40 mg/dL
- Triglycerides: less than 150 mg/dL
Other experts, including Dr. David Kessler, recommend even lower targets for LDL cholesterol, below 70 mg/dL, as a way to prevent heart disease.
Blood Pressure: Experts recommend a blood pressure of less than 130/80 mmHG. Keeping it below 120/80 is even better for supporting the health of your kidneys. Blood pressure can be measured at home with an arm cuff (which can be purchased online) as often as each day, or at your healthcare office. Ask your healthcare professional how often you should measure your blood pressure.
BMI (body mass index) and Waist Circumference: Excess weight can indicate an increased risk of heart disease. For many people who are affected by overweight or obesity, weight loss improves blood glucose management and lowers triglycerides, other measure of cholesterol, and blood pressure. These numbers can help you identify a healthy weight:
- BMI: 18.6 - 24.9 (you can measure BMI with an online calculator)
- Waistline: Smaller than 35 inches for women and 40 inches for men. Measure this with a measuring tape against your bare skin at belly button level.
Note: while BMI and waist circumference are great diagnostic tools and are widely used indicators of health, they do not tell the whole story, and they are most helpful when combined with other measurements (such as those described in this article).
Kidney function: Your heart and kidneys work together – they support each other! The kidneys help filter your blood and regulate blood pressure. If they are not working properly, the heart has to work harder. People with reduced kidney function or chronic kidney disease (CKD) are at increased risk of heart disease. Similarly, heart disease can cause pressure to build up in the kidney and lower its supply of oxygenated blood, which increases your risk of kidney disease.
There are two tests to measure kidney function. It is important to test kidney function with both tests every year, or as recommended by your healthcare professional.
- Estimated glomerular filtration rate (eGFR): this blood test is a measure of how well the kidneys are filtering the blood.
- eGFR above 60 is considered normal; however, eGFR below 89 may not mean complete kidney health, depending on your overall health
- eGFR lower than 60 may mean you have stage 3 moderate kidney disease
- eGFR of 15 or lower indicates unhealthy kidneys that may be close to kidney failure
- Albumin: this urine test measures how much albumin protein is present in the urine. The presence of protein in the urine can indicate that the kidneys are damaged.
- 30 mg/g or less is normal
- More than 30 mg/g may be a sign of kidney disease
Learn more about the relationship between diabetes, the heart, and the kidneys here.
Note: Many diagnostic measures, including eGFR, use factors of race and ethnicity to adjust a person's evaluation. These adjustments have no genetic or medical basis; they are rooted in discriminatory and outdated healthcare systems. Please ask your healthcare professional how adjustments to your eGFR may affect your diabetes care.
Improve your numbers:
There are several ways to improve heart health, whether or not you have heart disease.
Diet:
- Eat a healthy, balanced diet that supports stable blood glucose levels. In addition to our healthy and delicious recipes from Catherine Newman, we want to share some great recipes from KDBH (like fresh vegetable summer rolls, chopped veggie salad with feta, and mojo-marinated pork tenderloin).
- Eat fiber-rich foods, like vegetables – find our veggie-forward, plant-based recipes here.
- Avoid sugar and reduce carbohydrates, salt, and saturated fats. One way to accomplish this is to avoid highly processed or packaged foods. Read our recent article "Six Tips: How to Cut Sugar and Processed Foods from Your Diet."
- See diaTribe’s nutrition principles for more information.
Exercise:
- Adults should get:
- At least 150 to 300 minutes each week (2.5 to 5 hours, or 20 to 40 minutes per day) of moderate-intensity aerobic activity, like a brisk walk;
- At least 75 to 150 minutes each week (about 10 to 20 minutes per day) of vigorous aerobic exercise, like running or jogging; or
- Some combination of the two types of exercise.
- In addition, experts also strongly recommend lifting weights or doing some form of resistance training.
- Exercise helps the heart stay strong and slows the progression of heart disease.
- If you already have heart disease, talk with your healthcare team about safe ways to approach physical activity, such as walking. Read more about how Adam Brown has found walking to be extremely helpful with blood sugar management.
- Ask your healthcare professional if it would be helpful to lose weight.
Medications:
There are many medication options to help you improve your heart health. Recently, two classes of medications have been shown to protect the heart, as a critical added benefit to effectively lowering blood sugar and reducing weight and hypoglycemia: SGLT-2 inhibitors and GLP-1 agonists. KDBH has a valuable resource guide on medications that can help manage type 2 diabetes and improve heart health. Read up, and talk with your healthcare team about which options may be best for you.
The American Diabetes Association recommends that most people with type 2 diabetes, and many people with type 1 diabetes, should take statins to lower their LDL cholesterol for heart health. Similarly, blood pressure should be actively treated to meet your target.
The infographic below can help you learn more about what you can do to support a healthy heart. Click here to download the infographic.
