How To Keep Your Feet Healthy With Diabetes

Having diabetes along with years of high glucose levels can lead to problems with your feet. Know what foot conditions can develop, how to treat them, and ways to prevent them.
People with diabetes, particularly those who have dealt with higher than recommended blood glucose levels over a long period of time, are at increased risk for foot problems that range from corns and calluses to foot ulcers and amputations.
Following years of decreasing rates, the number of diabetes-related amputations is once again on the rise, according to the Centers for Disease Control (CDC). To help people with diabetes prevent and/or manage diabetes-related lower limb amputations, the CDC has resources on preventing diabetes-related amputations, recovering from a diabetes-related amputation, and managing diabetes-related amputations and mental health.
Thankfully, with a basic understanding of diabetes-related foot concerns, self-care suggestions that can keep your lower extremities healthy, and guidance on how to seek care for screening and prevention, you have the potential to keep your feet healthy for many years to come.
How diabetes-related foot problems begin
Most often, diabetes-related foot problems occur due to a combination of factors. A first problem could be as simple as an ingrown toenail or a barefoot walk on hot pavement. You may not feel the pain from a foot injury due to decreased sensation from peripheral neuropathy. The injury can quickly get worse before you notice and seek medical care.
Peripheral artery disease (PAD) leads to reduced circulation and blood flow in the lower limbs, which can increase the risk that a foot injury becomes infected. Treatment may require antibiotics or the need to refrain from walking for a period of time. Healing an infection can be arduous and time-consuming. If the wound does not heal, amputation may be recommended.
The good news? There are a number ways to prevent diabetes-related foot conditions, including regular foot care and keeping your glucose levels in range.
Common diabetes-related foot problems
The following are common problems for people living with diabetes foot complications:
-
Calluses: A build-up of layers of hard skin, typically on the bottom of the foot.
-
Corns: A build-up of layers of hard skin on or near a bone in the toes or between toes.
-
Dry skin: Rough skin that is prone to cracking and creates an opportunity for infection.
-
Fungal infection: Toenails that may change in color and thickness.
-
Diabetic peripheral neuropathy: Loss of sensation in the feet and lower extremities with or without pain due to high blood glucose over a long period of time.
-
Hammertoe: A toe that tends to curl under the foot due to the tendon from a weakened muscle becoming shorter. Surgery is sometimes required to straighten the toe.
-
Charcot foot: Nerve damage to joints and soft tissue in the foot that can cause the foot to develop an odd shape, known as a rocker bottom.
-
Diabetic foot ulcer: This is an open sore or wound that can develop from a simple scrape or crack in the skin.
-
Peripheral artery disease: A buildup of plaque on the walls of blood vessels that narrows the arteries, reducing blood flow in the feet and legs. PAD is most often diagnosed when there is pain in the legs and feet while walking.
Risk factors for foot problems
People with diabetes with one or more of the following are at higher risk for developing the foot problems mentioned above:
-
Consistently high glucose levels for many years
-
Established peripheral neuropathy with loss of protective sensation
-
History of foot ulcers or amputation
-
History of smoking or currently smoking
-
Foot deformities
-
Calluses or corns
-
Peripheral artery disease
-
Diabetic retinopathy or visual impairment due to diabetes
-
Chronic kidney disease (especially if requiring dialysis)
How to prevent or delay diabetes-related foot problems
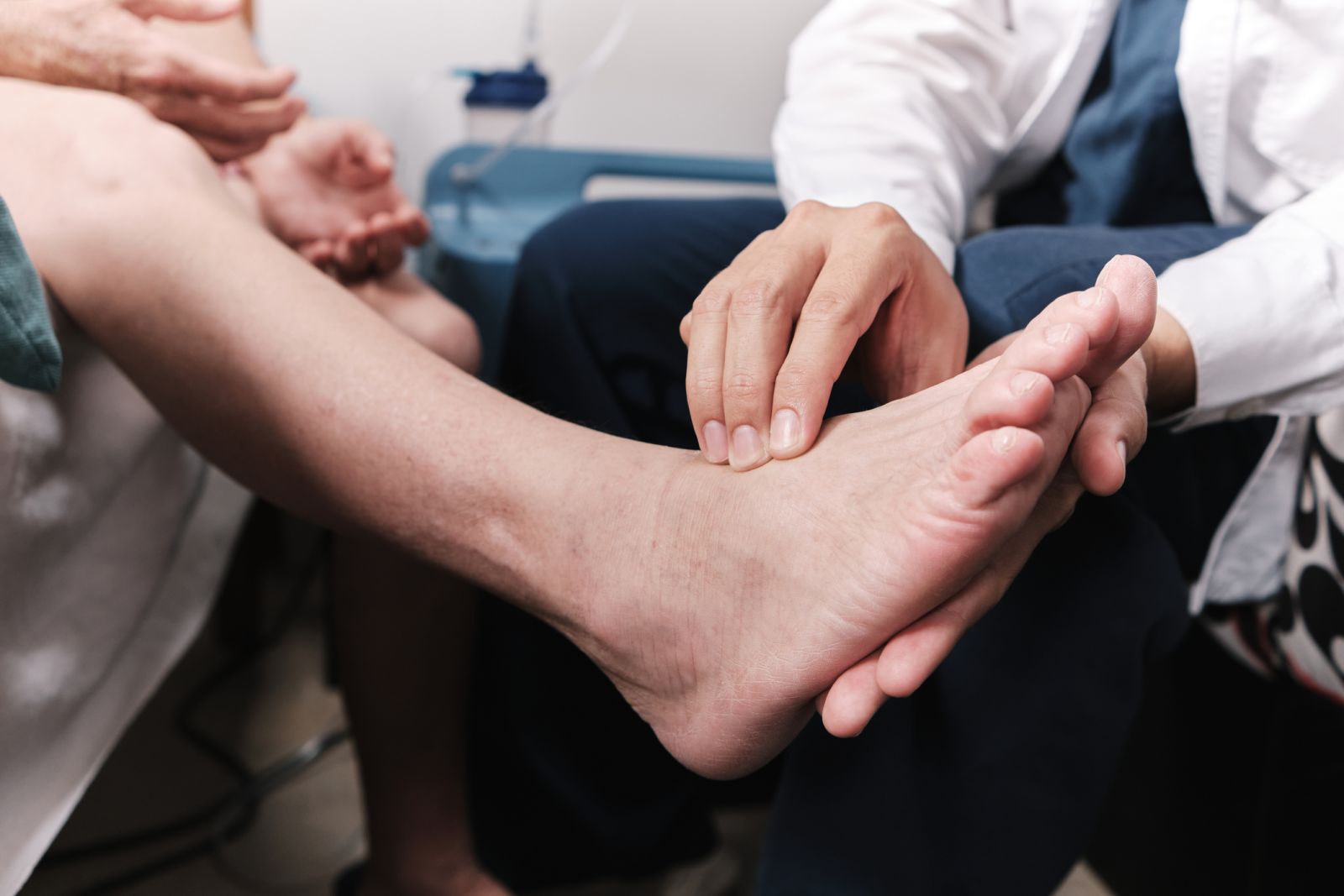 As is true for the prevention or delay of most diabetes-related complications, there are self-care actions to take daily like maintaining glucose, blood pressure, and lipids at target levels and keeping feet moisturized. There are also actions one should take annually – or more frequently, if need be – to screen for foot problems.
As is true for the prevention or delay of most diabetes-related complications, there are self-care actions to take daily like maintaining glucose, blood pressure, and lipids at target levels and keeping feet moisturized. There are also actions one should take annually – or more frequently, if need be – to screen for foot problems.
Clare Tuson, who has had type 1 diabetes for over 47 years, first learned about the importance of regular foot care in 2014 when she signed up to participate in a diabetes clinical trial. A nerve conduction velocity test used in the study diagnosed Tuson, who is an avid hiker and tennis player, as having peripheral diabetic neuropathy.
The experimental study drug, which required weekly injections, was ultimately unsuccessful, yet there was a silver lining.
“The diagnosis of diabetic peripheral neuropathy encouraged me to take better care of my diabetes and pay more attention to my feet,” she said.
In addition to checking her feet in the shower every day and wearing shoes that fit comfortably, Tuson asks her endocrinologist at routine visits to check her feet. In her experience, it's not been a regular part of the exam. Tuson also has access to a podiatrist (a foot doctor), whom she consults if she develops a foot problem.
Daily self-care behaviors
If you're told you have signs of diabetes-related neuropathy or reduced circulation in your lower legs and feet, here are some daily self-care behaviors to prioritize.
-
Keep glucose in a desired target range. Good glucose management over time can help reduce the risk of foot problems. Working with a diabetes healthcare provider can help determine your ideal glucose targets.
-
Do not smoke, or quit smoking. Smoking can reduce blood flow to the feet. A referral to a foot care specialist such as a podiatrist is recommended for people who smoke and have risk factors or signs of foot problems.
-
Inspect feet regularly: Get into a regular routine. Check between toes along with the surfaces of the foot. If you have reduced sensation, use a large mirror to look at your feet for problems. If you cannot check on your own, ask for help from a family member or friend. Look for cuts, sores, blisters, corns, calluses, or any redness.
-
Wash feet daily: Wash your feet regularly, making sure the water is not too hot (90-95 degrees F is safe). Avoid soaking your feet and be sure to dry them well. Rub a small amount of lotion or cream on the tops and bottoms to keep skin moist and healthy. Do not put lotion or cream between your toes, an area more prone to fungal infections. Sprinkle talcum powder or cornstarch between toes to keep the skin in those areas dry.
-
Smooth corns and calluses gently: Talk with a primary care provider or a podiatrist about how to deal with corns and calluses if they are frequent or problematic. Do not use scissors or other tools to cut them off. Using a pumice stone after bathing to gently rub the skin in one direction to smooth these down may be helpful.
-
Trim toenails straight across with a toenail clipper: Trim toenails after bathing, when nails are softer and easier to cut. Trim toenails straight across; this can help prevent ingrown toenails caused by rounding the corners of nails. Don’t cut too close, and avoid breaking any skin. File any sharp ends. If you have reduced sensation or can’t see or reach your toenails to cut them, find someone to do this for you or seek the help of a podiatrist.
-
Wear well-fitting shoes: Buy lightweight shoes that cushion the feet, distribute pressure evenly, have a broad and square toe box, and laces with 3-4 eyes per side and a padded tongue. Walking or athletic shoes are best. Avoid vinyl or plastic shoes and ones with pointed toes. Make sure there is room at the toes and around the sides. Break in new shoes slowly. If you have an existing foot problem, you may need extra wide or deep shoes. If this problem has caused a deformity in one or both of your feet, therapeutic shoes that are custom-molded to relieve pressure may be required. These may be covered by health insurance plans or Medicare.
-
Wear closed toe shoes and socks as often as possible: Avoid walking barefoot or without shoes. Wear socks with breathable fabrics that draw sweat away from your skin (cotton and special acrylic fibers – check the label for fabric that “wicks” sweat). There are special socks designed for people with diabetes, and socks that can monitor the temperature of your feet. Talk to a healthcare provider about these products before making a purchase if you’re unsure about what to buy.
-
Protect feet from temperatures that are too hot or cold: If you have reduced sensation in your feet, check the temperature of your skin with your fingers or an elbow. Wear shoes if the surface you walk on will be hot. Use sunscreen on your feet to avoid sunburns. Keep feet away from heaters and open fires. In cold weather, use socks and lined boots to keep your feet warm.
-
Keep blood circulation flowing: Put feet up on a stool rather than letting feet dangle or rest on the floor. Get up and move regularly. Wiggle your toes and roll your ankles around.
Annual (or as-needed) actions
If you detect symptoms of a foot problem, act quickly to have it evaluated – a small foot problem can rapidly become a big one. Contact a healthcare provider or podiatrist for a foot issue that is not healing or is getting worse. They can establish and put a treatment plan in place.
Get your feet checked at every healthcare visit. To make sure feet get examined, take your shoes and socks off when in the exam room and ask for a foot check to be done.
Ask your doctor to do a comprehensive foot exam at least once a year (people with neuropathy need more frequent foot exams). During the exam, make sure your provider does the following:
-
Asks about and looks for signs and symptoms of a foot problem
-
Makes a point to look at the skin on feet and lower legs as well as shape of the feet
-
Asks about developing a complete self-care routine for feet; this may include a referral to a foot care specialist such as a podiatrist
-
Feels skin for temperature or uses a pin to lightly prick skin on the legs, feet and hands to assess sensation
-
Checks pedal pulses (on the top of the foot or behind the ankle bone) to assess circulation
-
Uses a tuning fork that applies vibration on the skin to assess large fiber function
-
Uses a monofilament (a thin, stiff strand of nylon) on several points of the feet to determine if they have sufficient sensation or are at risk for problems due to lack of feeling
With a regular foot care routine, Tuson has managed to keep her feet in healthy condition.
“Having been diagnosed in the days of people having to do urine sugar testing and taking insulin made from pigs, I’m very grateful for the new technologies and products to help me live my best life,” Tuson said. “I realize it’s on me to keep my feet in good shape and live a healthy lifestyle.”
Recommendations in this article are aimed at adults with type 1 and type 2 diabetes and exclude children and adolescents as well as pregnant people with diabetes. Discuss your targets with your healthcare providers; recommendations may vary based on a number of personal factors.
About this series
Each year the American Diabetes Association updates its Standards of Medical Care in Diabetes based on current science. We’ve translated key points of the up-to-date Standards into plain English so you know how to stay healthy and minimize diabetes complications.
Additional reporting by Jeemin Kwon
Other articles in this series: