On Becoming A Therapist: Mental Health, Diabetes, and a New Chapter
By Adam Brown
 By Adam Brown
By Adam Brown
“In the beginner’s mind there are many possibilities; in the expert’s mind there are few.” - Shunryū Suzuki, Zen Mind, Beginner’s Mind
That quote, in all of its Zen beauty and paradox, wonderfully captures how I’ve been feeling of late.
Six months ago, I started on an exciting (and slightly terrifying!) new journey: returning to school to become a licensed therapist. Ultimately, I hope to combine everything I’ve learned in diabetes with a new set of skills in mental health, emotional well-being, and behavior change.
I’m a big believer in hitting the “reset” button and becoming a beginner again at many points in life. This is definitely one of those times. After almost 10 years writing about diabetes as a journalist, I felt it was time for a new challenge and a different way of thinking.
Diabetes tools have radically improved since I started at diaTribe in 2010, but living with a 24/7 chronic condition still means coping with thoughts, behaviors, emotions, difficult people, stress, shame, stigma, discrimination, and more. Understanding these topics is what becoming a therapist is all about – and there is a lot to absorb!
I’m learning about diagnoses like depression and anxiety, but also about family lifecycles, the teenage brain, racism, intergenerational trauma, and parenting styles – and how all of those things might layer on top of each other. In every class, I see clear connections to managing diabetes.
I’m learning about techniques used in psychotherapy, mental health, and counseling – approaches that have been used and studied for decades. I think they have a lot to offer people with diabetes.
-
How do I address unhelpful, negative thought patterns that keep repeating themselves? – Cognitive Behavioral Therapy (CBT) (article; book)
-
How do I cope with strong emotions, manage stress, live in the present, and accept unpredictability? – Dialectical Behavior Therapy (DBT; article; book), Acceptance & Commitment Therapy (ACT; article; book)
-
How do I deal with family conflict and relationship challenges? Family Therapy, Emotion-Focused Therapy (EFT; article)
-
How do I help someone change that seems totally uninterested in change? –Motivational Interviewing (article; book)
-
How do I use stories to understand a problem and find a new narrative? – Narrative Therapy (article)
-
How do I focus on solutions, rather than problems? – Solution-Focused Brief Therapy (SFBT; article; book)
All of this applies to diabetes! And this is another reason why I’m embarking on this journey: I see a huge need to bring more of these proven psychological tools, techniques, and principles into diabetes – technology, education, programs, language, healthcare offices, care delivery, and beyond. For example, I like to imagine what it’d be like if new continuous glucose monitor (CGM) prescriptions came with a short course on how to cope with the data from a behavioral, emotional, and mental health perspective. Product designs might change based on these principles. For instance, diabetes data might emphasize when things went well (Bright Spots!), so I might do more of that stuff.
Compared to the general population, people with diabetes have higher rates of depression, anxiety, panic disorder, sleeping challenges, and beyond. This is not surprising, considering the mental, emotional, and behavioral demands of diabetes – see the 42 Factors that Affect Blood Glucose Poster & booklet. I’m excited to see how the tools from the mental health field could be deployed in diabetes.
At the same time, there are so few mental healthcare professionals that specialize in diabetes. How do we scale the combination of expertise in both areas to reach more people? Moving in this new direction is one way I hope to contribute.
Q&A with the diaTribe team
Q: What books do you recommend for people interested in mental health?
In addition to the books noted above, these have had an impact on me recently:
Get Out of Your Mind and Into Your Life – A fantastic overview of Acceptance and Commitment Therapy (ACT). Some of my friends also recommend the shorter ACT Made Simple or The Happiness Trap.
Cognitive Behavioral Therapy Made Simple – I recommended this last year and stand by it! It’s a great overview of CBT – especially the negative automatic thoughts chapter.
Wasted: A Memoir of Anorexia and Bulimia – A gripping personal account of living with an eating disorder; I cried multiple times. There is a lot that applies to diabetes – food and family, eating behaviors, coping with trauma, our culture of thinness, and beyond.
Why Are All The Black Kids Sitting Together in the Cafeteria? – Powerful insights on race, why we don’t talk about it, and why that’s a big problem. This is definitely a book I will re-read.
On the pricier and geekier side, I thoroughly enjoyed these three textbooks:
Interviewing in Action in a Multicultural World – Focused on therapist skills and filled with great tips for healthcare providers. There was a whole chapter on therapist office setup!
Current Psychotherapies – A wonderful overview of the major schools of therapy.
Motivational Interviewing – A fantastic read on the change process. I loved all the therapy transcripts.
These two come highly recommended and are on my bookshelf, but I haven’t had a chance to read them quite yet:
The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma
The Gift of Therapy: An Open Letter to a New Generation of Therapists and Their Patients
Q: Have you learned anything about the benefits of mindfulness/meditation practices that could be actionable? Any other stress management practices?
Yes! Mindfulness practices are widely used in many schools of therapy – DBT, ACT, Mindfulness-based CBT, Mindfulness-Based Stress Reduction (MBSR), Gestalt therapy, etc. They are incorporated often into class – e.g., to get into the present moment, to notice thoughts without judgment, to get in touch with emotions, feelings, and bodily sensations. Mindfulness is an important therapist skill, given the emotionally challenging nature of what we do.
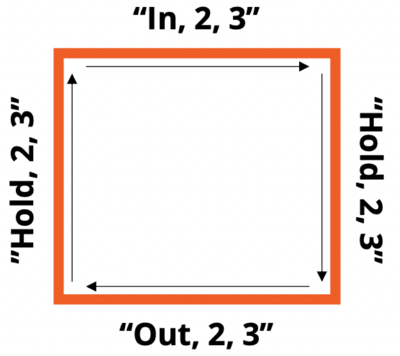
I tend to be very cognitive in my approach to life and problem solving, so I’ve been trying to deepen my mindfulness practice. I still use Waking Up and Calm. I’ve also been using square breathing quite a lot, which only takes 2-3 minutes. The diagram below illustrates the exercise: breathe in for three seconds, hold for three seconds, exhale for three seconds, hold for three seconds. The part in quotes is meant to be said in your head. Repeat the square at least five times. (I often use a longer 4-second interval.) This can also be used on walks, as each side of the square can be synchronized with a step.
Q: Who are some people doing interesting mental health projects?
I’m excited about the EMBARK study – a major trial that is now recruiting to test an intervention for diabetes distress. It involves some of the leading diabetes psychologists. Read more in our Trial Watch!
Q: Any other concepts or ideas that have had a big impact on you so far?
Understanding the difference between individuals and the context that surrounds them. Most of my diabetes writing and thinking has focused on my individual experience – decisions, thoughts, tools, how I respond to situations, etc. These are important, but they are only a sliver of the complete mental health picture.
These graphics from some of my class readings illustrate context:
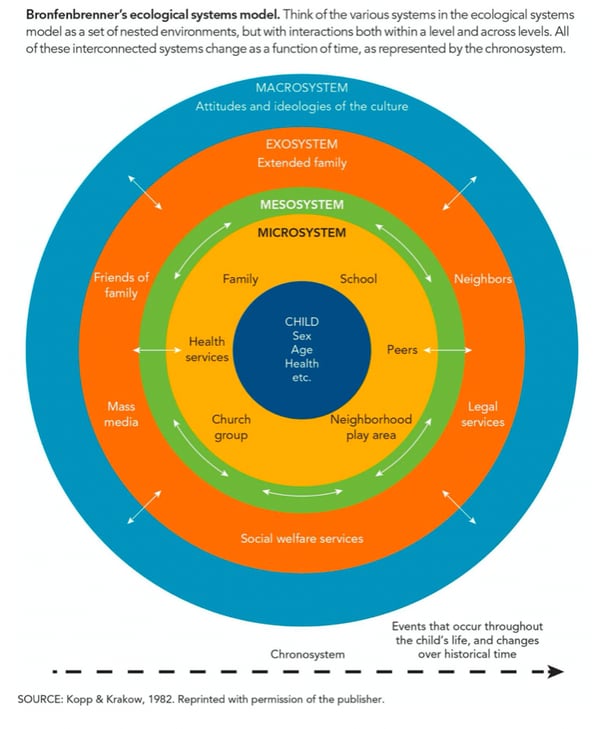
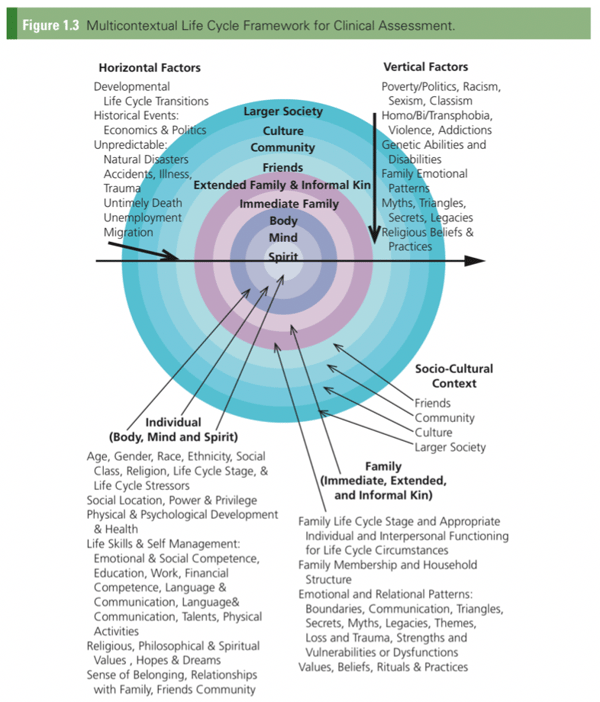
Source: The Expanding Family Life Cycle: Individual, Family, and Social Perspectives by Monica McGoldrick, Nydia Garcia Preto, and Betty Carter
I like these graphics, as they highlight how an individual in the middle circle is surrounded by a whole lot of context and systems. They are intentionally complicated; that is reality!
What I find most staggering about these diagrams is to think of all this context in combination with the 42 Factors That Affect Blood Glucose, most of which reside in that narrow center.
As a person living with diabetes, I have been shaped by my particular family history, my racial/ethnic identity, my socioeconomic situation, my neighborhood, my school and work environments, the popular culture, this moment in history, and beyond. Much of this isn’t in my control, but it still influences my mental health, how I approach diabetes, how much time I have for self-care, my access to tools, and my support system. Context changes radically throughout life and varies a lot from person-to-person. It is important to understand context, because it can inform a treatment focus.
As a therapist in training, I’m learning to better appreciate these critical contextual factors – zooming out from an individual to the context and systems around them. It is another way I’m learning to see many possibilities. I have found that this awareness has a way of building humility and empathy and reducing instincts to judge or blame. When someone irritates me in daily life, I now try to pause and think of a much longer list of why they might be acting a certain way.
Our program also strongly encourages finding a personal therapist while we’re studying in school – another journey I’m starting on now. It’s inevitable that something from my past will come up in the room with a client, and if I haven’t dealt with my own issues, it is that much harder to help others.
Q: How is your role at diaTribe changing?
I’m transitioning to a guest contributor role after several years here as a Senior Editor. This position has been one of the greatest honors of my life – to read and learn so much, to meet many incredible people, and to have the opportunity to share ideas in writing. You can still reach me at this diaTribe email, and I’m happy to answer follow-up questions from the content shared above.
I’ve also recently joined the team bringing Tidepool Loop to market – an automated insulin delivery app for iPhone that I deeply believe in. I will continue to write and advocate as much as I can.
May You Find Bright Spots!
very best,
Adam







